On Monday, the Equal Employment Opportunity Commission (EEOC) released final rules on how employers can offer workers financial incentives of up to 30% of the cost of their cheapest health insurance plans to participate in wellness programs without violating federal laws protecting the confidentiality of medical information. The ruling aims to clear up confusion over the way two federal laws protecting employees’ medical privacy apply to the popular programs, which are designed to control medical spending by reducing obesity, smoking, and other risk factors.
First, some background information. The 2010 Affordable Care Act (ACA) allowed U.S. employers to increase the rewards they offer to employees who participate in wellness programs. However, in a series of lawsuits against companies, including Honeywell, the EEOC said requests for medical information related to incentive-based wellness programs violated the Americans with Disabilities Act or the Genetic Information Nondiscrimination Act. As a result of these lawsuits and ambiguity in the conflicting regulations, the EEOC sought opinions and comments in order to provide clarity on the regulatory framework governing certain types of wellness programs. Many employees, including those involved in the lawsuits, felt that the incentives were so high that they amounted to penalties for those who do not want to participate.
Under the new rules, incentives for wellness programs are open only to employees, not their families. The new rules are more restrictive than those passed under the ACA, which allowed incentives of up to 30% of the actual cost of an employee’s insurance plan and 50% for approved programs (only smoking-cessation programs received that approval).
Rather than get into the debate of whether or not large incentives operate more like penalties, the questions and commentary below are designed to bring up several issues with these programs regardless of where one stands on the incentive vs. penalty argument.
Is Honeywell A Winner?
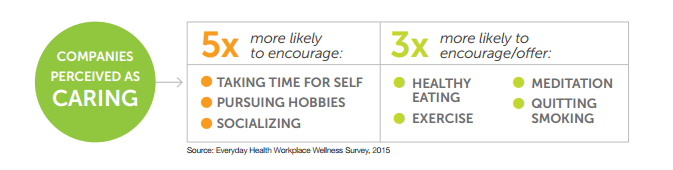
From a legal perspective, the ruling certainly looks like a win, although the lawsuit was essentially thrown out already (the Federal court in Minnesota declined the motion for injunction but didn’t rule on the merits of the case). From a business strategy perspective, one could easily argue that Honeywell is still the loser. The goal of successful businesses is to move toward their strategic vision, which often includes higher revenue and more profits. To make progress towards this goal, the best companies rely on talent. No matter how you measure it, having employees involved in a lawsuit against your company over one of the most important benefits you offer them (healthcare) is never good. A recent Global Wellness Institute report showed that “caring companies” boost worker health and productivity, not wellness programs. Employers that are perceived as caring by their employees have a better talent pool to accomplish their goals.
Why Are Employers Still Obsessed With Ineffective Wellness Solutions?
Health risk assessments and biometric screenings are the focal points for this ruling. Employees that don’t want to share private medical information with their employers are forced to choose between losing a large incentive or participating in the program against their will. Why are employers so willing to put employees into this challenging situation? It would make more sense if these programs led to a healthier workforce, but given the large body of research that suggests they do not, it is odd that employers would go to such lengths to force participation in ineffective programs.
If An Employers Wellness Program Is So Great, Why Are They Considered Involuntary?
If the program is truly going to help employees live healthier and happier lives, there wouldn’t need to be a huge incentive to drive participation. The reality is that employees have seen the research about how HRAs and screenings do not work, and combined with their skepticism of their employers’ interest in their health, employees are in no rush to participate.
Why Premium Differentials?
Most of the lawsuits use premium differentials as part of the program in question. A study from the Perelman School of Medicine at the University of Pennsylvania shows that although many employers provide financial incentives in the form of premium differentials for weight loss, these programs are largely ineffective. Premiums differentials don’t work because of the large timing gap in behavior and reward and many employees don’t see it directly because it shows up as an adjustment on their paychecks. It is odd how employers still default to spending their incentive dollars in areas that are the least effective.













