Fourteen percent of the U.S population is now enrolled in a consumer-driven health plan (CDHP) and another 14% is enrolled in a high-deductible health plan (HDHP). Because of the low-premium and high-deductible nature of these options, members are more likely to show cost-conscious behaviors than those of traditional plans, according to a report from the Employee Benefit Research Institute.
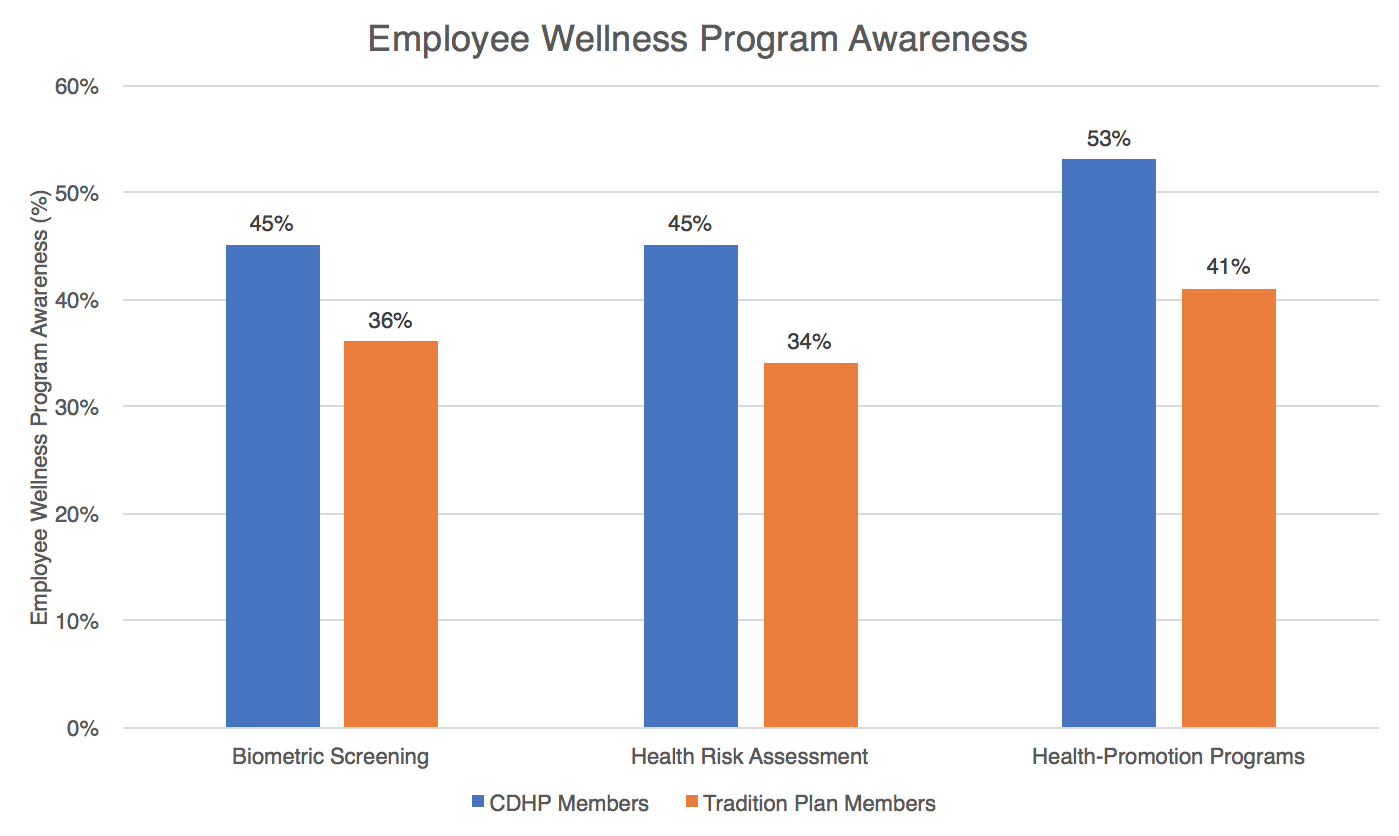
Some of the cost-saving behaviors are greater interest in employee wellness programs and an increase in awareness in the plan offerings. Specifically, “45% of CDHP enrollees reported that their employer offered a health risk assessment, compared with only 34% of traditional-plan enrollees.” Similarly, 53% of CDHP enrollees reported being aware of health-promotion programs at their organization, compared to 41% for their traditional-plan counterparts. Overall, the awareness of and participation in health and wellness program are much higher among CDHP enrollees than members of traditional health plans
Another trend kindled by the popularity of high-deductible healthcare is the growing interest in health savings accounts (HSAs). On this front, employers are taking an active role in helping their employees, reportedly contributing more in both frequency and dollar amount to HSAs than in the past. “78% of CDHP enrollees reported that their employer contributed the account in 2016, up from 67% in 2014.”
Organizations can use this information to hone their approach to delivering more effective and engaging wellness programs. For example, employers can help employees offset the higher deductibles by offering HSA contributions for engaging in wellness activities. One Wellable partner, HSA Health Plan, is seeing success with this model of incentivizing healthy behavior through HSA contributions. Through Wellable’s customizable and configurable platform, HSA Health Plan members can earn $20 a month deposited into their HSA by taking at least 8,000 steps in 20 or more days in the month.